Health
New Surgical Robotic System Set to Transform the Future of Surgery and Patient Care
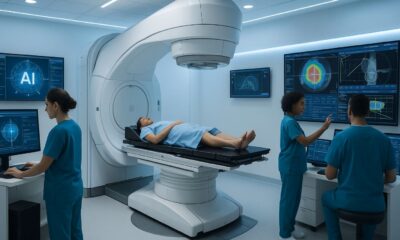
The University of the Free State (UFS) and the Free State Department of Health mark a transformative moment in healthcare with the launch of the Versius Surgical Robotic System – the first of its kind in Southern Africa.

The University of the Free State (UFS) and the Free State Department of Health are not just introducing new technology, but embarking on a journey that will revolutionize surgery and patient care in the region. This is the message delivered by MaQueen Letsoha-Mathae, Premier of the Free State, during the official launch of the Versius Surgical Robotic System on 11 March 2025 at the UFS Faculty of Health Sciences. The Free State is now the first region in Southern Africa to implement this technology, having successfully completed nine robotic-assisted surgeries at Universitas Academic Hospital within the last month.
The successful procedures, which took place between 24 February and 6 March, included complex surgeries such as radical prostatectomies and cholecystectomies, demonstrating the Versius system’s potential to improve patient outcomes. Prof Freddie Claassen, Academic Head of the Department of Urology at UFS and Universitas Hospital, was among the first surgeons from the university to be trained on the system and use it in operations.
A Significant Milestone
“This moment marks a significant milestone not only for our beloved Free State, but for the entire health-care landscape in Southern Africa. We are not merely launching a new technology; we are embarking on a journey that will transform the future of surgery and patient care in our province and beyond,” said Letsoha-Mathae.
She emphasized that the introduction of the Versius Surgical Robotic System aligns with the Free State’s vision to become a hub of healthcare innovation and excellence in Southern Africa. “With this groundbreaking system, we are not only enhancing surgical precision, but also significantly improving patient outcomes,” Letsoha-Mathae added.
The Versius Surgical Robotic System is known for its versatility and adaptability, seamlessly integrating into any operating room. It can be used in high-specialty procedures, including thoracic, colorectal, general and upper gastrointestinal, hernia, gynaecology, and urology surgeries.
Prof Hester C. Klopper, Vice-Chancellor and Principal of UFS, reflected on the role of the university in shaping the future of healthcare. “This moment is not just a technological milestone, but a symbol of what we can achieve as an institution when we unite academic excellence, visionary leadership, and a commitment to community impact with partners in the private sector and government,” she said.
She stressed that the launch reaffirms UFS’s ongoing dedication to academic excellence, technological innovation, and societal impact, while addressing some of the most pressing healthcare challenges both regionally and globally. “Versius is an investment in the well-being of our communities and an essential step towards bridging the healthcare gap in our region,” said Prof Klopper.
Enhancing Surgical Precision
Prof Vasu Reddy, Deputy Vice-Chancellor of Research and Internationalisation at UFS, explained the significant benefits of robotic-assisted surgeries. “Robots such as the Versius system are tools that enhance the senses and skills of surgeons during delicate operations. Unlike traditional surgery, which requires large incisions, robotic surgery enables doctors to perform operations with smaller cuts, reduced pain, and less scarring,” he said.
Robotic surgery improves surgical outcomes by allowing for greater precision, accuracy, and reduced chances of complications. “The robots do not tire, they do not lose focus, and they can handle repetitive tasks with ease, making the entire process safer for patients,” Prof Reddy continued. He further highlighted the role of AI and robotics in healthcare, emphasizing that human innovation and machine precision together can elevate the standard of care.
According to Premier Letsoha-Mathae, the Versius Surgical Robotic System represents a significant leap towards enhancing healthcare delivery in Southern Africa. “The benefits of Versius are profound: patients will experience quicker recoveries and an earlier return to work, ultimately leading to a healthier, more productive society,” she said.
The system’s modular and scalable design ensures that it can be integrated into operating rooms with minimal infrastructure changes, making it accessible across both private and state healthcare sectors. This adaptability promises to expand access to robotic-assisted surgery, helping to bridge the gap in healthcare delivery.
Through the collaboration between the Department of Health and UFS, the launch of the Versius Surgical Robotic System is a testament to the shared commitment to addressing regional and global healthcare challenges. It also underscores the importance of continuing innovation and academic excellence in advancing healthcare technology and patient care.
Health
Need to Shift Cancer Care Towards Early Detection in India: Keith Flaherty
If cancers are identified at an earlier stage, therapies can be far more effective and, in many cases, curative, Flaherty says

India needs to place greater emphasis on early cancer detection to improve treatment outcomes, internationally renowned oncologist Keith Flaherty said during a visit to VPS Lakeshore Hospital in India’s southern state Kerala.
“Early detection is absolutely essential to better treatment outcomes. If cancers are identified at an earlier stage, therapies can be far more effective and, in many cases, curative,” Flaherty said after launching Lakeshore Yathra, an initiative focused on wellness and early cancer detection across Kerala.

Flaherty, Director of Clinical Research at the Massachusetts General Hospital Cancer Center and Professor at Harvard Medical School, spoke about the future of cancer care and the evolution of precision medicine since 2000. He said India has significant potential to contribute to precision oncology and targeted cancer therapies, but noted that important gaps remain in understanding the molecular profile of cancers among the Indian population.
Widely recognised for his contributions to precision medicine and targeted cancer therapy, Flaherty’s work has played a major role in shaping modern oncology globally.
Presiding over the event, S.K. Abdulla, Managing Director of VPS Lakeshore Hospital, said healthcare institutions must increasingly focus on wellness, prevention and early diagnosis alongside treatment.
“Through Lakeshore Yathra, we are trying to take healthcare closer to people and encourage regular screening and timely identification of disease. Detecting cancer early can make a significant difference in treatment outcomes and quality of life,” he said.
Abdulla also highlighted the hospital’s collaboration with the Indian Dental Association for a statewide initiative aimed at improving early oral cancer detection. The programme focuses on training dentists across Kerala to identify suspicious lesions and ensure timely referrals.
Moni Abraham Kuriakose, Head of the Institute of Head & Neck Sciences at VPS Lakeshore Hospital, said the hospital is adopting a three-pronged strategy for early cancer detection.
“Yathra includes screening programs for patients and family members visiting the hospital, population-level outreach initiatives for cancer and non-communicable disease screening in partnership with NGOs and workplaces, and the deployment of a mobile medical unit to facilitate diagnostic investigations closer to patients’ homes,” Moni said.
Flaherty also interacted with doctors and healthcare professionals during the event and shared insights on evolving approaches in oncology care, cancer research and precision medicine.
Health
Lancet Commission Launched to Tackle Health and Justice Impacts of Rising Sea Levels
A new Lancet Commission will examine how rising sea levels impact health, equity, and global systems, with experts calling it an urgent crisis.

A new global commission led by The Lancet has been launched to examine the growing health and justice impacts of sea-level rise, as climate change accelerates risks for millions living in coastal and low-lying regions.
The Lancet Commission on Sea-Level Rise, Health and Justice, announced on April 8, brings together 26 international experts to assess how rising seas are reshaping public health, livelihoods, and global equity.
A Growing Crisis Beyond Climate
Sea-level rise, driven by anthropogenic climate change, is already contributing to displacement, food and water insecurity, and changing patterns of infectious diseases. The Commission marks the first major effort to analyse these intersecting risks through a health-focused lens.
“This commission comes at exactly the right time… sea-level rise is no longer a distant threat. It is already disrupting lives, health and wellbeing, especially for the most vulnerable,” said Christiana Figueres, Co-Chair of the Commission and a former UN climate chief.
Experts warn that the impacts extend far beyond environmental damage, affecting the social and economic fabric of vulnerable communities.
“Rising seas don’t just threaten coastlines, they threaten lives, livelihoods, and basic fairness. This is not only a climate problem. It is a health crisis, a justice crisis, and an urgent call for collective action,” said Jemilah Mahmood, Commissioner, Lancet Commission, and Executive Director of the Sunway Centre for Planetary Health, Malaysia.
An Urgent Global Health Challenge
The Commission is supported by the WHO Asia-Pacific Centre for Environment and Health and aims to generate evidence-based policy recommendations to strengthen adaptation, resilience, and equitable responses.
Dr Sandro Demaio, Director of WHO ACE, emphasised the immediacy of the crisis.
“Sea-level rise is no longer a distant threat — it is a public health emergency unfolding now. Through this WHO supported global Commission, we are clear: inaction is not neutral, it is a choice that puts lives and justice at risk.”
Human Impacts at the Core
The Commission also highlights the disproportionate burden on vulnerable populations, particularly in coastal and low-income regions.
“Rising sea levels are more than an environmental issue; they quietly contaminate water, displace communities, and increase health risks for those least able to cope. Every centimetre of sea level rise is not just a measure of water, but a measure of injustice,” said Kathryn Bowen, Co-Chair of the Commission.
A Defining Policy Moment
With projections suggesting that hundreds of millions of people could be displaced by the end of the century, the Commission aims to inform global policy and strengthen international cooperation.
“Sea-level rise is not just an environmental issue — it is a test of our commitment to people, equity, and future generations,” said Jiho Cha, Member of Parliament, Republic of Korea and Co-Chair of the Commission.
The Commission will contribute to global policy discussions, including international climate platforms, and aims to place human and planetary health at the centre of climate action.
Health
Researchers Develop AI Method That Makes Computer Vision Models More Explainable
A new technique developed by MIT researchers could help make artificial intelligence systems more accurate and transparent in high-stakes fields such as health care and autonomous driving by improving how computer vision models explain their decisions.

MIT researchers have developed a new explainable AI method that improves the accuracy and transparency of computer vision models, helping users trust AI predictions in healthcare and autonomous driving.
Researchers at MIT have developed a new approach to make computer vision models more transparent, offering a potential boost to trust and accountability in safety-critical applications such as medical diagnosis and autonomous driving.
In a media statement, the researchers said the method improves on a widely used explainability technique known as concept bottleneck modeling, which enables AI systems to show the human-understandable concepts behind a prediction. The new approach is designed to produce clearer explanations while also improving prediction accuracy.
Why explainable AI matters
In areas such as health care, users often need more than just a model’s output. They want to understand why a system arrived at a particular conclusion before deciding whether to rely on it. Concept bottleneck models attempt to address that need by forcing an AI system to make predictions through a set of intermediate concepts that humans can interpret.
For example, when analysing a medical image for melanoma, a clinician might define concepts such as “clustered brown dots” or “variegated pigmentation.” The model would first identify those concepts and then use them to arrive at its final prediction.
But the researchers said pre-defined concepts can sometimes be too broad, irrelevant or incomplete for a specific task, limiting both the quality of explanations and the model’s performance. To overcome that, the MIT team developed a method that extracts concepts the model has already learned during training and then compels it to use those concepts when making decisions.
The approach relies on two specialised machine-learning models. One extracts the most relevant internal features learned by the target model, while the other translates them into plain-language concepts that humans can understand. This makes it possible to convert a pretrained computer vision model into one capable of explaining its reasoning through interpretable concepts.
“In a sense, we want to be able to read the minds of these computer vision models. A concept bottleneck model is one way for users to tell what the model is thinking and why it made a certain prediction. Because our method uses better concepts, it can lead to higher accuracy and ultimately improve the accountability of black-box AI models,” Antonio De Santis, lead author of the study, said in a media statement.
De Santis is a graduate student at Polytechnic University of Milan and carried out the research while serving as a visiting graduate student at MIT’s Computer Science and Artificial Intelligence Laboratory (CSAIL). The paper was co-authored by Schrasing Tong, Marco Brambilla of Polytechnic University of Milan, and Lalana Kagal of CSAIL. The research will be presented at the International Conference on Learning Representations.
Concept bottleneck models have gained attention as a way to improve AI explainability by introducing an intermediate reasoning step between an input image and the final output. In one example, a bird-classification model might identify concepts such as “yellow legs” and “blue wings” before predicting a barn swallow.
However, the researchers noted that these concepts are often generated in advance by humans or large language models, which may not always match the needs of the task. Even when a model is given a fixed concept set, it can still rely on hidden information not visible to users, a challenge known as information leakage.
“These models are trained to maximize performance, so the model might secretly use concepts we are unaware of,” De Santis said in a media statement.
The team’s solution was to tap into the knowledge the model had already acquired from large volumes of training data. Using a sparse autoencoder, the method isolates the most relevant learned features and reconstructs them into a small number of concepts. A multimodal large language model then describes each concept in simple language and labels the training images by marking which concepts are present or absent.
The annotated dataset is then used to train a concept bottleneck module, which is inserted into the target model. This forces the model to make predictions using only the extracted concepts.
The researchers said one of the biggest challenges was ensuring that the automatically identified concepts were both accurate and understandable to humans. To reduce the risk of hidden reasoning, the model is limited to just five concepts for each prediction, encouraging it to focus only on the most relevant information and making the explanation easier to follow.
When tested against state-of-the-art concept bottleneck models on tasks including bird species classification and skin lesion identification, the new method delivered the highest accuracy while also producing more precise explanations, according to the researchers. It also generated concepts that were more relevant to the images in the dataset.
Still, the team acknowledged that the broader challenge of balancing accuracy and interpretability remains unresolved.
“We’ve shown that extracting concepts from the original model can outperform other CBMs, but there is still a tradeoff between interpretability and accuracy that needs to be addressed. Black-box models that are not interpretable still outperform ours,” De Santis said in a media statement.
Looking ahead, the researchers plan to explore ways to further reduce information leakage, possibly by adding additional concept bottleneck modules. They also aim to scale up the method by using a larger multimodal language model to annotate a larger training dataset, which could improve performance further.
This latest work adds to growing efforts to make AI systems not only more powerful, but also more understandable in domains where trust can be as important as accuracy.
-

 Society5 months ago
Society5 months agoThe Ten-Rupee Doctor Who Sparked a Health Revolution in Kerala’s Tribal Highlands
-

 Society5 months ago
Society5 months agoFrom Qubits to Folk Puppetry: India’s Biggest Quantum Science Communication Conclave Wraps Up in Ahmedabad
-

 Space & Physics5 months ago
Space & Physics5 months agoIndian Physicists Win 2025 ICTP Prize for Breakthroughs in Quantum Many-Body Physics
-

 Sustainable Energy6 months ago
Sustainable Energy6 months agoThe $76/MWh Breakthrough: Battery-Backed Solar Becomes the Cheapest Firm Power
-

 Society5 months ago
Society5 months agoWhy the ‘Stanford Top 2% Scientists’ Label Is Widely Misrepresented
-

 Space & Physics5 months ago
Space & Physics5 months agoWhen Quantum Rules Break: How Magnetism and Superconductivity May Finally Coexist
-

 Space & Physics5 months ago
Space & Physics5 months agoAncient Martian Valleys Reveal Gradual Climate Shift From Warm And Wet To Cold And Icy: Study
-

 Earth5 months ago
Earth5 months agoClimate Disasters Cost the World Over $120 Billion in 2025, New Report Finds